ACCESS Model: From data collection to measurable outcomes
The conversation around wearable data in healthcare is evolving. For years, the focus has been on collecting more data, building dashboards, and increasing user engagement.
But the ACCESS Model signals a shift.
After analyzing it, one thing becomes clear:
it’s not just about collecting data anymore.
It’s about proving outcomes with that data.
From activity tracking to outcome validation
Most digital health products today are still built around:
Dashboards
User engagement metrics
Feature expansion
These elements are important, but they are no longer enough.
The ACCESS Model raises the bar. It pushes companies to demonstrate measurable impact, not just activity. This means showing how data translates into real improvements in health outcomes.
That is a fundamentally different challenge.
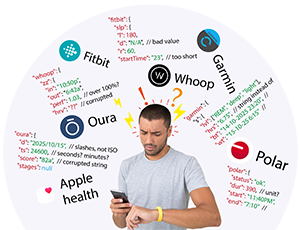
The hidden challenge: data inconsistency
At first glance, this shift may seem like a product or analytics problem. In reality, it is a data problem.
Wearable data comes from multiple devices, each with:
Different formats
Different methodologies
Different definitions for the same metrics
For example, sleep, HRV, or activity scores are not calculated the same way across devices.
Without consistency, it becomes difficult to:
Compare users
Generate reliable reports
Prove outcomes
And under the ACCESS Model, that becomes a critical limitation.
Why infrastructure matters more than ever
This is where many teams run into friction.
If your data is not:
Consistent
Comparable
Structured
then everything that comes after, from analytics to reporting, becomes more complex.
The ACCESS Model makes one thing clear:
data infrastructure is no longer optional.
It is the foundation for:
Reliable reporting
Clinical validation
Scalable product development
Without it, even the best product experience cannot deliver measurable results.
Data quality over data quantity
A common instinct is to collect more data.
But more data does not solve the problem if the data is fragmented.
The real priority shifts to:
Clean data
Standardized metrics
Reliable pipelines
In other words:
Data quality > Data quantity
This principle becomes essential when outcomes need to be validated, not just displayed.
What this means for digital health teams
For teams building in digital health, wearables, or remote monitoring, the implications are clear:
Product strategy must align with outcome measurement
Data pipelines must support consistency across devices
Infrastructure decisions become strategic, not just technical
This is not just a technical evolution.
It is a shift in how products are evaluated.
Where solutions like ROOK fit
To meet these new expectations, teams need tools that simplify complexity.
Platforms like ROOK help unify and normalize data from multiple wearable devices, making it easier to work with structured, comparable health data.
This allows teams to focus less on data fragmentation and more on building products that can actually demonstrate impact.
Final thoughts
The ACCESS Model is not about adding more features.
It is about raising the standard.
From tracking to proving.
From engagement to outcomes.
From data collection to data reliability.
The teams that adapt to this shift will be better positioned to build scalable, data-driven healthcare solutions.
Because in this new model, success is not measured by how much data you have—
but by what you can prove with it.
Learn More: