Wearable and Blood Test Data Integration: Building a Complete View of Health
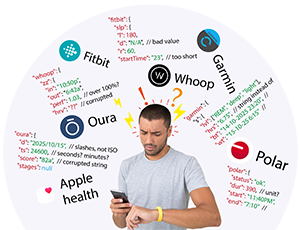
Health data is becoming increasingly rich, but also increasingly fragmented.
On one side, wearable devices provide continuous, real-time signals about activity, sleep, heart rate, and recovery. On the other, blood tests offer precise, clinical snapshots of what is happening inside the body at a biochemical level.
Individually, both are valuable. But when combined, they unlock a much more powerful capability: a holistic, longitudinal view of health.
In this article, we explore how integrating wearable data with blood test data enables better insights, stronger products, and more informed decision-making.
Two types of health data: continuous vs. clinical
Understanding the difference between these data sources is key.
Wearable data (continuous signals)
Wearables capture behavioral and physiological trends over time, including:
heart rate and HRV
sleep patterns
activity levels
stress indicators
recovery metrics
This data is:
continuous
high-frequency
context-rich
It answers: How is the body behaving day to day?
Blood test data (clinical snapshots)
Blood tests provide biochemical measurements, such as:
glucose and HbA1c
cholesterol (LDL, HDL, triglycerides)
hormones
inflammatory markers
micronutrients
This data is:
periodic
precise
clinically validated
It answers: What is happening inside the body at a molecular level?
Why integration matters
Separately, each dataset has limitations.
Wearables provide trends but lack clinical depth
Blood tests provide accuracy but lack continuity
When combined, they create context + precision.
Example
A wearable detects elevated resting heart rate and low HRV
A blood test shows increased inflammation markers
Together, this provides a stronger signal than either alone.
Key use cases
Personalized health insights
Combining both data sources allows platforms to:
correlate lifestyle behaviors with biomarkers
provide more accurate recommendations
track how interventions impact health
For example:
linking sleep quality to glucose regulation
understanding how activity affects cholesterol trends
Preventive health and early detection
Integration enables earlier detection of risks by:
identifying deviations in wearable trends
validating them with lab results
triggering timely interventions
This is especially valuable for:
metabolic health
cardiovascular risk
chronic condition management
Longevity and optimization platforms
Longevity-focused products rely on:
continuous tracking (wearables)
periodic validation (blood tests)
This allows users to:
measure progress over time
test interventions (nutrition, training, supplements)
optimize long-term health strategies
Insurance and underwriting
For insurers, combining both datasets enables:
more accurate risk models
dynamic underwriting
behavior-linked incentives
This creates a shift toward data-driven and preventive insurance models.
Technical challenges in integration
While the opportunity is strong, integration is not trivial.
Data fragmentation
Wearables and lab providers operate in different ecosystems:
different APIs
different data formats
different update frequencies
Lack of standardization
Metrics are not always directly comparable:
wearable HRV vs clinical measurements
different units and reference ranges in labs
Normalization is required to make data usable.
Temporal alignment
Wearable data is continuous, while blood tests are periodic.
To extract value, systems must:
align timelines
detect meaningful correlations
avoid false interpretations
Data quality and reliability
Both sources have limitations:
wearable accuracy varies by device
lab results depend on timing and conditions
Combining them requires careful validation.
Privacy and compliance
Handling combined datasets increases sensitivity.
Companies must ensure:
secure data handling
user consent management
compliance with regulations (HIPAA, GDPR)
The role of data infrastructure
To make integration scalable, companies need the right infrastructure.
This includes:
unified APIs for wearable data
structured ingestion of lab results
normalization layers
analytics and interpretation models
Some platforms in the ecosystem are already working on simplifying wearable data integration, enabling developers to focus on building health experiences instead of managing multiple device connections.
From data to decision-making
The real value of integration is not in the data itself, but in what it enables.
Effective systems should:
combine signals into clear indicators
highlight meaningful changes
provide actionable recommendations
adapt over time
For example:
“Your recovery is decreasing and inflammation markers are elevated — consider reducing training load and improving sleep consistency.”
The future: multi-layer health data platforms
The next generation of health platforms will not rely on a single data source.
They will combine:
wearable data
lab results
medical records
lifestyle inputs
This creates a multi-layer health data stack capable of supporting:
personalized medicine
preventive care
continuous health optimization
Final thoughts
Wearables and blood tests represent two complementary views of health:
one continuous and behavioral
the other precise and clinical
Individually, they are powerful. Together, they are transformative.
As integration improves, we will move from tracking data to understanding health, and ultimately to guiding decisions.
The companies that succeed will be those that can connect, standardize, and translate these data sources into meaningful, actionable insights.